Project REVERE
Readiness Evaluation via Electrophysiology, Radiology, and Evidence
A longitudinal neurological surveillance platform for Special Operations Forces
Background: A Critical Healthcare Challenge
Special Operations Forces operators experience repeated blast exposure at rates above the general military population. A 2024 study in the Proceedings of the National Academy of Sciences examined 30 active-duty US SOF personnel with an average of 17 years of service and found that higher cumulative blast exposure was associated with alterations in brain structure, brain function, and neuroimmune markers, as well as lower quality of life [1]. No signs of injury were identified by conventional MRI. The findings required 7 Tesla functional MRI, Connectome-grade diffusion MRI, and PET imaging [1,2]. The damage is real, it accumulates, and standard clinical imaging does not catch it.
Diffuse axonal injury is considered a signature wound of mild TBI, but standard CT cannot detect it [3]. Cognitive screens detect impairment only after symptoms appear. Self-report is unreliable because operators have strong career incentives to under-report symptoms. No single modality is sufficient. What the field needs, and has not had, is a multimodal longitudinal system that tracks each operator against their own baseline across a full career.
Our Solution: Six-Modality Surveillance With Agentic Per-Operator Tracking
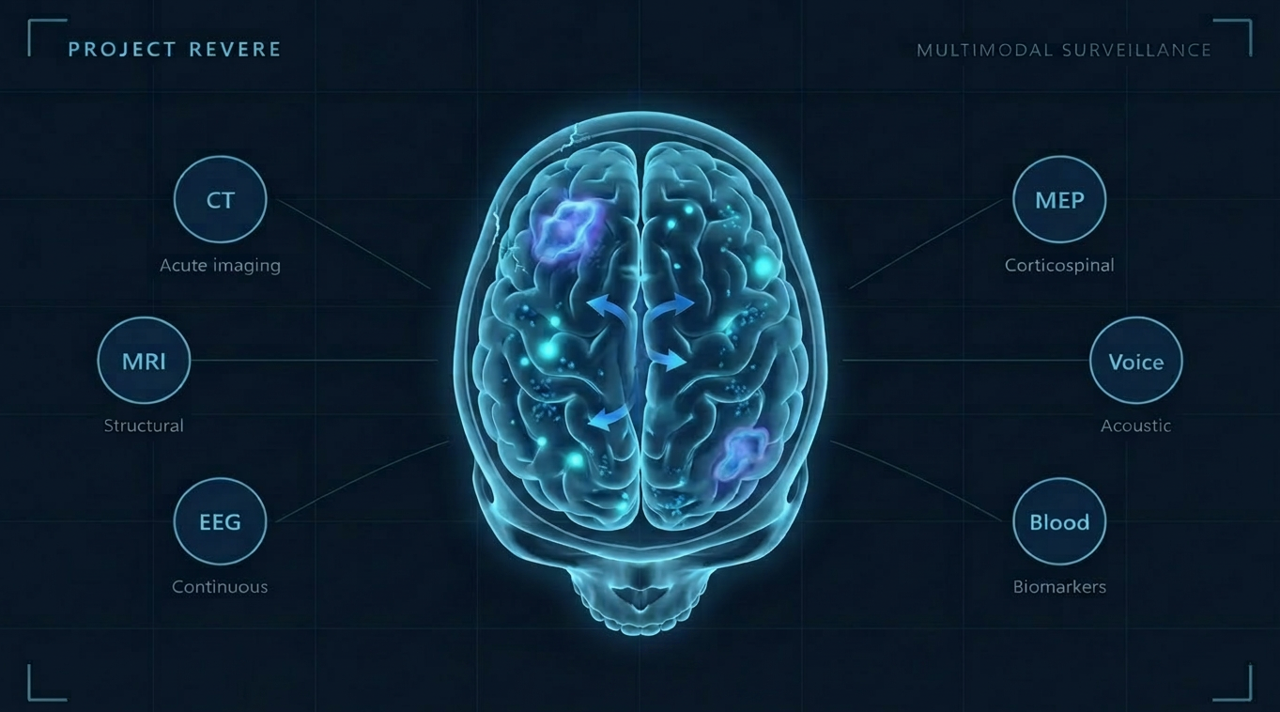
Project REVERE integrates six imaging, physiology, and fluid biomarker modalities, each doing the job it is actually good at, wired together by a per-operator agentic AI that monitors each operator's personal trajectory across their full time in service.
CT handles event-triggered hemorrhage and fracture rule-out, anchored on our quantum-classical hybrid model that achieves 93.6% F1 on subdural hemorrhage detection trained on the public CT-ICH dataset. MRI provides the structural and functional ground truth at baseline and periodic checkpoints, extracting trajectory signal across the feature classes identified in the peer-reviewed SOF blast literature [1]. EEG is the continuous longitudinal backbone, portable and repeatable at a unit medical facility, architecturally consistent with our PTSD severity detection system (greater than 96% accuracy) and Alzheimer's detection system (90.86% accuracy, 98.35% AUC). MEP testing adds a quantitative probe of corticospinal tract integrity, with peer-reviewed evidence that MEP amplitudes and latencies change after mild TBI and concussion [4,5], and directly extends our MS progression prediction methodology that achieved 6-fold risk stratification on longitudinal evoked potential data. Voice analysis uses our AI-powered communication platform, which captures and reproduces a person's own voice from 30 seconds of recording at 95.42% classification accuracy, to establish a personal acoustic baseline at enrollment and measure every subsequent speech sample against that fingerprint rather than a population mean. Blood biomarkers combine the FDA-cleared Abbott i-STAT TBI test for acute post-event screening [6,7] with longitudinal panels of neurofilament light chain, GFAP, tau, and p-tau181, each of which has peer-reviewed evidence of elevation after blast exposure on different timescales [8,9].
The trajectory engine fuses all six modalities into a per-operator longitudinal model. A persistent AI agent assigned to each operator holds their full neurological history, monitors incoming assessments against their personal baseline rather than a population average, and produces a readiness output that is auditable at the unit and command level.
Why This Matters
For Special Operations Command: Commanders see trajectory, not snapshots. The stack runs on portable, edge-deployable hardware with no cloud dependency. Routine follow-up visits run under an hour at a unit medical facility. The platform does not require new hospital-grade hardware acquisition, because it integrates data from infrastructure VA medical centers and major military treatment facilities already have.
For Operators: Assessment is anchored to the operator's own baseline, not a population mean. That matters because it catches decline in high-performing individuals who would still score above population norms even after real cumulative injury. Voice preservation at enrollment serves a second purpose beyond diagnostics: if an operator is later injured in a way that affects speech, their own voice is already preserved and can be restored through the same platform we originally built for ALS patients. The system is designed to be operator-protective first and command-visible second.
References
[1] Stone JR, et al. Impact of repeated blast exposure on active-duty United States Special Operations Forces. PNAS 121(18):e2313568121, 2024.
[2] Massachusetts General Hospital Center for Neurotechnology and Neurorecovery. Press release, April 22, 2024.
[3] Bryden DW, Tilghman JI, Hinds SR. Blast-Related Traumatic Brain Injury: Current Concepts and Research Considerations. Journal of Experimental Neuroscience 13, 2019.
[4] Livingston SC, et al. A preliminary investigation of motor evoked potential abnormalities following sport-related concussion. Brain Injury 24(6), 2010.
[5] Miller NR, et al. Acute and longitudinal changes in motor cortex function following mild traumatic brain injury. Brain Injury 28(10), 2014.
[6] FDA. K234143 Substantial Equivalence Determination for i-STAT TBI Cartridge with the i-STAT Alinity System, 2024.
[7] Bazarian JJ, et al. Serum GFAP and UCH-L1 for prediction of absence of intracranial injuries on head CT (ALERT-TBI). Lancet Neurology 17(9), 2018.
[8] Boutté AM, et al. Elevated Axonal Protein Markers Following Repetitive Blast Exposure in Military Personnel. Frontiers in Neuroscience, 2021.
[9] Graham NSN, et al. Poor long-term outcomes and abnormal neurodegeneration biomarkers after military traumatic brain injury: the ADVANCE study. Journal of Neurology, Neurosurgery & Psychiatry, 2025.